人和宠物的“耐药性”,其实是一条绳上的蚂蚱
如果你觉得抗生素“越来越不管用”,这可能并不是错觉。耐药性,正在悄悄改变我们对抗感染的方式。而很多人不知道的是——宠物,也在这条耐药性的链条之中。
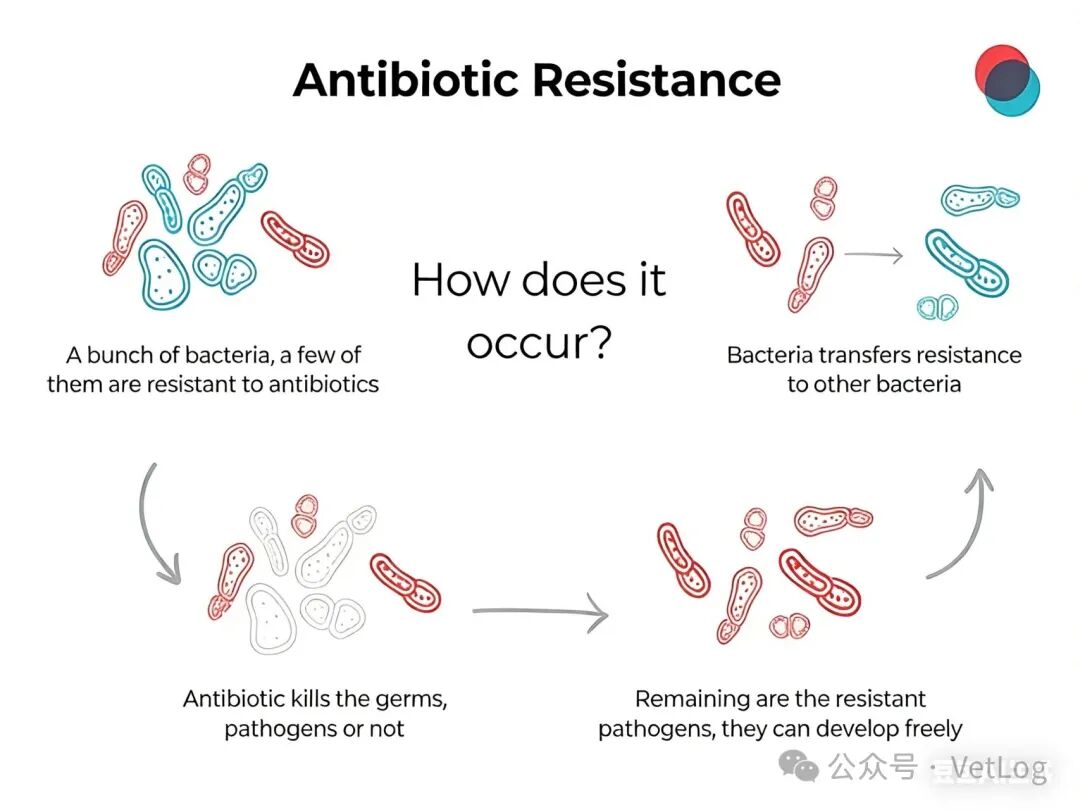
什么是耐药性?细菌为什么会“变聪明”?
抗生素并不是让人体产生免疫,而是直接杀死或抑制细菌。但当抗生素被反复、过度或不规范使用时,部分细菌可能存活下来,并逐渐获得“对药物不敏感”的能力。
这些“幸存者”会繁殖,把耐药基因一代代传下去,甚至还能通过质粒等方式把耐药性“分享”给其他细菌。久而久之,原本简单的感染,可能就需要更强的药物,甚至无药可用。
宠物用的抗生素,和人真的没关系吗?
事实上,兽医和人医使用的抗生素高度重合。青霉素类、头孢类、氟喹诺酮类等药物,既可能出现在医院,也可能出现在动物诊所。
当宠物出现皮肤感染、泌尿道感染或呼吸道疾病时,抗生素往往是重要的治疗手段。但如果:
• 没有明确诊断就用药
• 为了“保险”而过度使用
• 症状好转就提前停药
就可能在宠物体内“筛选”出耐药细菌。
人和宠物之间,细菌并不分界
在日常生活中,人和宠物的接触远比我们想象得频繁:
• 抚摸、拥抱、亲吻
• 清理猫砂盆、遛狗
• 共用沙发、床铺和生活空间
这些行为本身没有问题,但也意味着——细菌可以在人和宠物之间双向传播。已有研究发现,一些耐甲氧西林金黄色葡萄球菌(MRSA)等耐药菌株,可以在人和宠物身上同时存在。
这并不是说“宠物不安全”,而是提醒我们:耐药性不是某一个物种的问题,而是一个共同面对的风险。
从家庭到社会:耐药性如何被放大?
除了家养宠物,畜牧业中的动物同样大量使用抗生素,用于治疗疾病、预防感染,甚至在部分地区用于促进生长。如果监管不严,耐药细菌可能通过:
• 肉类和奶制品
• 粪便进入环境
• 水源和土壤扩散
最终回到人类社会,形成一个难以切断的循环。
为什么耐药性是“慢性危机”?
与突发传染病不同,耐药性的发展往往是缓慢而隐蔽的。它不会立刻引发恐慌,却可能在未来导致:
• 常见感染变成“难治病”
• 手术、化疗等医疗操作风险上升
• 医疗成本显著增加
正因如此,世界卫生组织已将抗生素耐药性列为全球最严重的公共健康威胁之一。
我们能做什么?普通人并非无能为力
应对耐药性,不只靠医生和兽医,每个养宠家庭都可以参与:
• 不自行给宠物使用抗生素
• 严格遵循兽医的用药方案和疗程
• 不把人用抗生素“分给”宠物
• 通过疫苗、卫生管理和定期体检减少感染发生
预防感染,本身就是减少耐药性的最好方式。
一体健康:把人、动物和环境放在同一张图里
如今,科学界提出了“一体健康(One Health)”理念,强调:
人类健康、动物健康和环境健康是相互依存的整体。
对宠物负责任地用药,不只是关心它们的健康,也是在为整个社会的未来医疗安全做贡献。
当你下一次抱起自家毛孩子时,不妨记住:
在对抗耐药性这场长期战役中,人和宠物是站在同一阵线的伙伴。 🐾💊
(部分图片来自于网络,如果侵权请联系删除)